A promising blood test could potentially predict the early stages of Alzheimer’s disease long before symptoms appear. Researchers from Mass General Brigham in the US have discovered that a blood biomarker known as pTau217 might serve as an early indicator of hazardous amyloid-beta and tau protein build-ups in the brain.
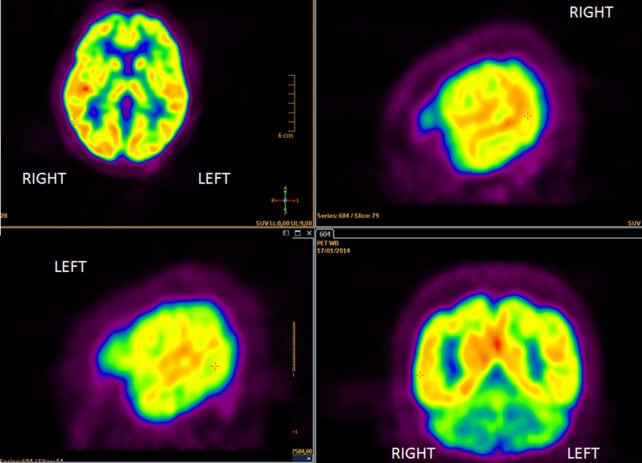
These protein accumulations have been associated with Alzheimer’s for some time. Currently, PET (positron emission tomography) brain scans are often used to detect these signs. There is a possibility that pTau217 blood tests could identify high-risk Alzheimer’s cases even earlier.
“We used to think that PET scan detection was the earliest sign of Alzheimer’s disease progression, revealing amyloid accumulation in the brain 10 to 20 years before symptoms appear,” says lead author Hyun-Sik Yang, a neurologist at Mass General Brigham. “But now we are seeing that pTau217 can be detected years earlier, well before clear abnormalities appear on amyloid PET scans.”
The study involved 317 participants aged between 50 and 90, all cognitively healthy at the start, and tracked over an average of eight years. Data from amyloid-beta and tau PET scans, cognitive testing, and pTau217 levels in blood tests were collected, combined, and monitored over time.
The results showed that blood tests closely matched PET scans for detecting protein tangles and clumps. In some instances, rising pTau217 levels predicted changes even before they were visible on brain scans.
The researchers found that high pTau217 levels were linked to the future development of Alzheimer’s, while low levels indicated a minimal risk of the disease. “What stood out in our study is that even when amyloid scans appear normal in the clinic, the pTau217 biomarker can identify individuals who later become amyloid-positive,” says Yang. “It also shows that those with low pTau217 levels are likely to stay amyloid-negative for several years.”
Elevated pTau217 levels were also associated with a higher risk of cognitive decline during the study, mainly among those who had initial signs of toxic amyloid-beta protein build-up.
This new research supports previous studies suggesting that pTau217 in blood could be a valuable tool for predicting Alzheimer’s risk, serving as a biological marker that indicates abnormal brain activity.

However, it may take some time before this test is available in clinics. Researchers aim to gather more data to refine prediction algorithms, which will require larger and more diverse groups of volunteers.
Another challenge is that even if blood tests can accurately predict amyloid-beta or tau protein build-ups, these may not necessarily lead to dementia. Currently, doctors use a variety of tests and assessments to diagnose Alzheimer’s, as there is no single test that can definitively predict the risk years or decades in advance.
“As the field is evolving quickly, we’re excited to see discoveries on the research side being rapidly translated to clinical application,” says neurologist Jasmeer Chhatwal from Mass General Brigham. “By anticipating who’s going to turn amyloid-positive in the future, we are trying to push back the clock to enable earlier Alzheimer’s disease prediction.”
The research has been published in Nature Communications.