Recent research has uncovered a possible brain connection that may clarify why Tourette syndrome frequently coexists with other neuropsychiatric disorders, such as obsessive-compulsive disorder (OCD), potentially paving the way for improved treatments.
A team from Kobe University in Japan employed a mouse model exhibiting tic-like behaviors to examine the brain circuitry responsible for the involuntary movements associated with Tourette’s.
“We believe that the neuronal circuit we found plays a crucial role as a bridge connecting brain regions that were previously thought to act independently from each other,” says neurophysiologist Yoshihisa Tachibana, from Kobe University.
Using neuron-tracing techniques, researchers identified an active pathway between the brain’s major movement-control area, the basal ganglia, and the insular cortex, a key emotion-processing center.
Significantly, this pathway traverses the thalamus, a critical relay station in the brain, specifically through the intralaminar thalamic nuclei, which are responsible for directing neuron activity to its appropriate destinations.
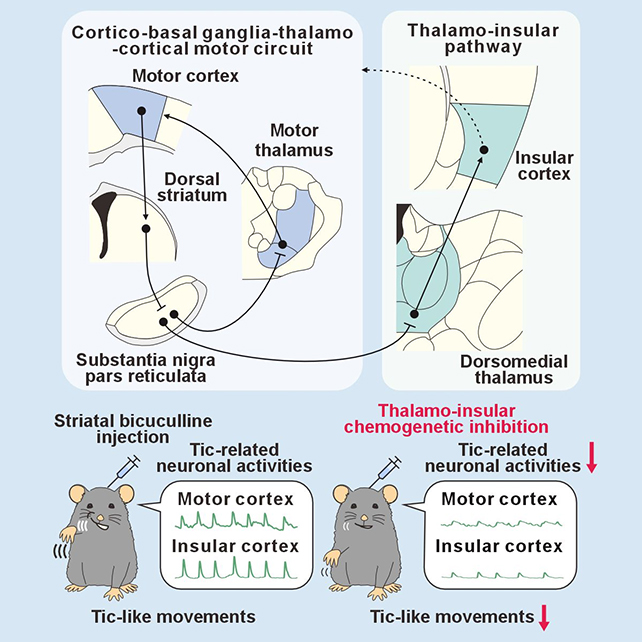
The researchers blocked the connection between the thalamus and insular cortex using a custom drug, which resulted in a significant reduction in the intensity of the tics in mice while also dampening related brain signals, highlighting the importance of this pathway.
Previous research had indicated the involvement of the insular cortex, a brain region connected to OCD, in Tourette’s and its possible link to involuntary tics, but the exact neural pathways transmitting these disrupted signals had not been established.
Another study found that a dental mouthguard designed to activate jaw muscles could alleviate Tourette’s tics through the insular cortex. These findings partly inspired the current research, which aims to explore more ways to target the neural connections involved.
Tourette syndrome and OCD frequently co-occur, along with other neuropsychiatric disorders like autism and ADHD, suggesting interconnected brain regions.
 frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>
frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>Tourette’s is also associated with ‘premonitory’ mental urges that precede tics and are usually relieved by them, indicating that the syndrome is not solely about movement.
This discovery in brain wiring suggests that abnormal motor signals might spread into areas involved in emotional processing, potentially explaining the overlap between Tourette’s and other conditions.
“Abnormal insular cortex activity in patients with Tourette syndrome may contribute not only to motor symptoms such as tics but also to premonitory urges and comorbid psychiatric disorders, including OCD, ADHD, and ASD,” the team writes.
“However, because rodents cannot report premonitory urges, the present model should be interpreted as capturing selected features of tic-like behaviors.”
Gaining a deeper understanding of these brain processes might aid in developing future treatments. Deep brain stimulation of the thalamus is currently used to treat severe Tourette’s, although the mechanism of its effectiveness was not fully understood.
“Tic disorders, such as Tourette syndrome, are among the most common neuropsychiatric conditions and have a significant impact on children’s lives,” says Tachibana.
“However, their underlying neuronal mechanisms remain poorly understood.”

Each new study on Tourette’s and OCD contributes to a more comprehensive understanding of the fundamental brain activities involved and explains why unexplained urges and involuntary actions occur.
It will take time to determine how this brain relay hub can be manipulated to control the thoughts and movements associated with Tourette’s, as this specific brain link has only recently been discovered. However, there is significant potential.
One potential approach involves calming the basal-ganglia-to-insular-cortex pathway using ultrasound, which could help control tics. Nonetheless, this research must progress beyond mouse models to include human patients.
Related: Several Psychiatric Disorders Share The Same Root Cause, Study Suggests
“The currently used deep brain stimulation is invasive and comes with a risk of complications,” says Tachibana.
“On the other hand, targeted intervention of the neuronal processing in the circuit we identified, such as ultrasound neuromodulation, may be options for the development of less invasive and safer treatment methods.”
The research has been published in Cell Reports.