Weight loss medications like Wegovy can both positively and negatively affect the body. However, users might experience an unexpected side effect unrelated to physical health: social stigma.
Recent research indicates that individuals who lose weight using GLP-1 drugs face harsher judgment compared to those who slim down through diet and exercise. The findings may not be surprising, but they highlight an underlying issue.
Alarmingly, the study reveals that the stigma associated with using weight loss drugs can, in some cases, be more severe than the criticism faced by those who don’t lose weight at all. This could deter individuals from starting or continuing their medication, as the study authors caution.
“We anticipated some stigma around using a GLP-1,” says Erin Standen, the first author and a social psychology researcher at Rice University. “But the extent of it was surprising.”
 frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>
frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>Standen, along with researchers from the Mayo Clinic and the University of California, Los Angeles, conducted two randomized online experiments involving 1,313 adults in the US. Participants were asked to evaluate various character traits of a fictional 38-year-old based on their weight history.
The participants were given different narratives to assess their perceptions. These stories varied in the method of weight loss—either using GLP-1 drugs or through diet and exercise—and whether the weight loss was maintained, with some characters depicted as not having lost weight at all.
GLP-1 users were judged more negatively on most metrics compared to those who lost weight through diet and exercise. Study participants viewed GLP-1 users as lazier, less healthy, less disciplined, and less desirable to spend time with, as measured by participants’ willingness to associate with them.
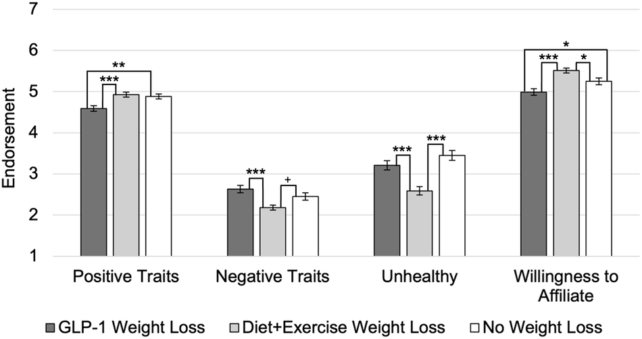
While GLP-1 users and those who did not lose weight received similar negative ratings, GLP-1 users were scored lower on positive attributes such as honesty and generosity. Additionally, those who had not lost weight were considered more desirable to spend time with than GLP-1 users.
“GLP-1 users faced social penalties not only compared to those who lost weight through diet and exercise,” Standen notes. “They were also judged more harshly than those who didn’t lose weight at all.”
In another experiment, participants rated weight regain after using GLP-1 drugs similarly to weight regain after diet and exercise. Both groups were viewed more negatively than characters who maintained their weight loss.
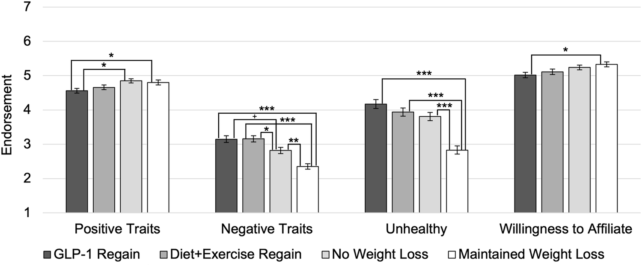
“What we’re observing is that individuals may encounter judgment at various stages,” Standen states. “They might be judged for their weight and their chosen method of managing it.”
While the study is limited to fictional characters described in brief bios, the results offer valuable insights.
Research on GLP-1 drugs, named after the glucagon-like peptide-1 hormone that helps regulate blood sugar, has shown that weight often returns quickly once the medication is stopped. This poses challenges in maintaining a healthy weight, which is crucial for reducing the risk of health issues related to obesity, including cardiovascular diseases, cancer, and depression.

The researchers are eager to shift perceptions around GLP-1 drugs, which are sometimes seen as an “easy way out” for those dealing with obesity or being overweight. Public opinion holds significance here.
“If individuals feel criticized for their health decisions, it can impact their willingness to take action,” Standen explains. “It can influence their pursuit of care, their openness with healthcare providers, and their overall health management.”
Related: Immune Cells ‘Remember’ Obesity Long After Weight Loss, Study Finds
Effective treatment for obesity can be transformative for those affected, and the study’s findings may contribute to public health messaging.
“As these treatments become more mainstream, understanding the social aspects is essential,” Standen states.
The study has been published in the International Journal of Obesity.





