Chronic pain has long been linked to depression.
Approximately 40% of adults with chronic pain exhibit clinical symptoms of depression. However, not everyone with chronic pain develops depression, prompting researchers to question why this occurs and what happens in the brain. Understanding this could pave the way for preventing depression.
Our recent publication in Science indicates that the answer lies within the brain.
In our study, we examined neuroimaging brain scans from 14,462 participants in the UK Biobank cohort. We compared those with chronic pain for at least seven years who did not exhibit symptoms of depression with those who did develop depressive symptoms.
For the latter group, depressive symptoms were either consistent throughout the seven years or developed after two or four years, allowing for an analysis of depression development related to chronic pain through brain imaging.
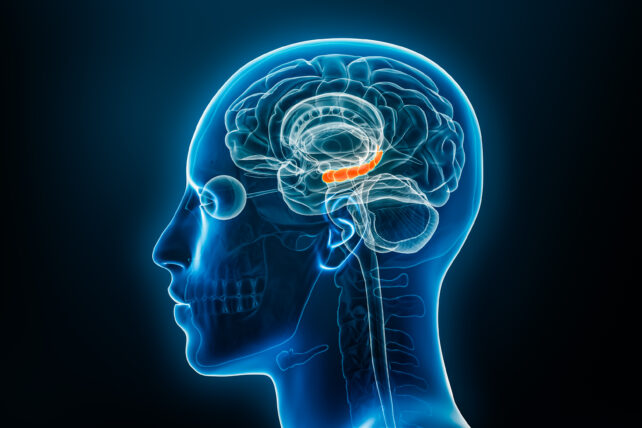
These neuroimaging studies revealed significant changes in the brain, particularly in the hippocampus, a structure crucial for learning and memory.
Participants with chronic pain but no depressive symptoms displayed modest increases in hippocampal volume and improved memory performance, suggesting a brain adaptation to pain stress.
Conversely, those with both chronic pain and depression showed reduced hippocampal volume and diminished cognitive performance. Further analyses suggested these changes occurred progressively, indicating the hippocampus may initially adjust to ongoing pain but becomes vulnerable over prolonged periods.
Notably, these patterns were consistent across various types of chronic pain, including back, stomach, knee, hip pain, and headaches, indicating the findings were not exclusive to one condition.
We further explored these brain changes using rodent models. The research showed a similar series of changes in hippocampal volume in animals, with initial cognitive improvements followed by anxiety-like behavior, eventually leading to depression-like symptoms and memory decline.
The hippocampus has been known to be involved in emotional memories and is highly susceptible to chronic stress. Its plasticity, or ability to form new nerve cells, is crucial in managing chronic stress.
Chronic stress has also been linked to increased apoptosis (nerve cell death) and reduced adult neurogenesis, the formation of new nerve cells in the hippocampus.
We identified the dentate gyrus region of the hippocampus as a critical regulatory hub in the transition from chronic pain to depression. Newly generated neurons in this area initially showed increased activity, indicating a protective response to pain. Over time, however, immune cells called microglia became abnormally activated, disrupting normal neural signaling in the hippocampus.
This abnormal activation marked the point where the brain’s protective response to pain began to fail.
Significantly, treatment with the antibiotic minocycline reduced abnormal microglial activation and depression-like behavior in animal models, preserving hippocampal structure and cognitive function.
Treating Pain and Depression
Our research suggests treatments like minocycline could help prevent depression in those with persistent pain, especially if administered early.
Other psychosocial, socio-economic, and genetic factors also influence pain perception, potentially exacerbating chronic stress and pain experiences.
However, there are evidence-based methods to reduce depression risk. A collaborative study by Fudan University and the University of Cambridge found that seven healthy lifestyle factors, including good sleep, exercise, and diet, could lower depression risk by 57%. These lifestyle factors were also linked to increased hippocampal volume, aligning with our study.

Mindfulness training, which emphasizes staying present and minimizing distractions, can also enhance working memory and increase hippocampal density.
A recent review indicated that experts in mindfulness meditation exhibit increased brain grey matter, including in the hippocampus. This training was shown to enhance hippocampal volume.
Mindfulness practice has been beneficial for improving life quality, not just in managing chronic pain, but also in reducing stress and depression symptoms.
Related: Chronic Pain Has 9 Distinct Types, According to a Large New Body Mapping Study
Our research has provided a crucial insight into why some individuals with chronic pain develop depression. It highlights the significant role of the hippocampus and suggests potential treatments to prevent depression in chronic pain sufferers.
The mechanisms we discovered in the brain may also apply to other conditions involving chronic stress, such as psychological trauma.![]()
Barbara Jacquelyn Sahakian, Professor of Clinical Neuropsychology, University of Cambridge; Jianfeng Feng, Professor of Science and Technology for Brain-Inspired Intelligence/ Computer Science, Fudan University; Trevor Robbins, Professor of Neuroscience, University of Cambridge, and Xiao Xiao, Associate Professor, Institute of Science and Technology for Brain-Inspired Intelligence, Fudan University
This article is republished from The Conversation under a Creative Commons license. Read the original article.





