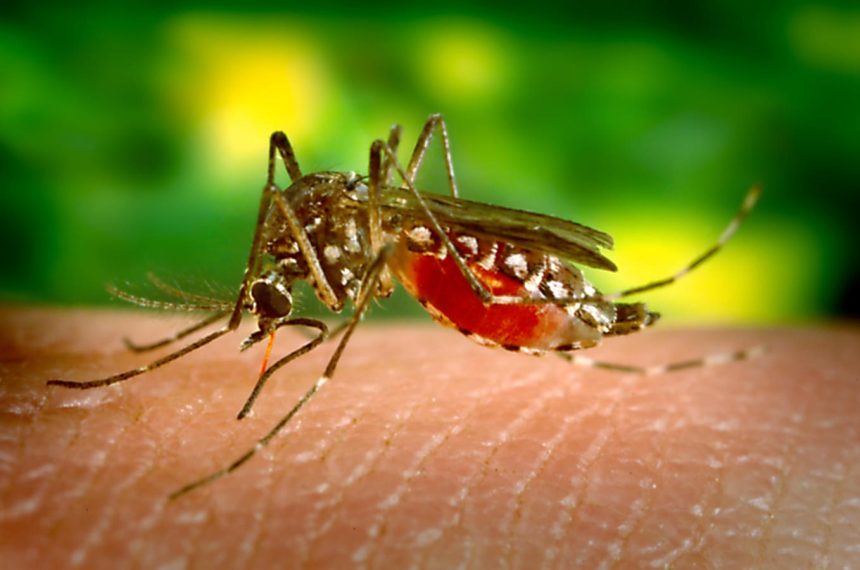
Female Aedes aegypti mosquito, a carrier of the Dengue fever, feeding on the human skin, 2005. Image courtesy Centers for Disease Control (CDC) / James Gathany. (Photo by Smith Collection/Gado/Getty Images)
Getty Images
For the last hundred years, mosquito-borne illnesses like dengue, malaria, and yellow fever have primarily affected tropical regions, not the continental U.S. However, this is shifting. Florida began encountering local dengue cases over a decade ago. In 2023, Texas and Florida reported local malaria cases. A recent paper in the CDC journal Emerging Infectious Diseases highlights a significant seven-week dengue transmission chain in Los Angeles County.
In the fall of 2024, fourteen individuals in LA County contracted dengue. Eight cases were concentrated within a mile in the San Gabriel Valley, while the other six were spread across five neighborhoods over 20 miles apart, likely introduced by travelers.
The southern U.S. is on the edge of suitable conditions for vector-borne diseases. Mosquitoes are present, and the climate is warm enough at times. Infected travelers frequently arrive. Previously, conditions were barely inadequate to sustain local transmission chains of dengue. The LA outbreak demonstrates what occurs when conditions become slightly favorable, even for a short period.
Timeline and geographic distribution of 14 locally acquired dengue cases, Los Angeles County, August–November 2024. Source: Vaughan et al., Emerging Infectious Diseases 32(5), 2026.
CDC
What Seven Weeks Means
Dengue involves a transmission cycle where a mosquito bites an infected person, the virus multiplies in the mosquito over eight to twelve days, and then the mosquito bites another person. This new host incubates the virus for five to seven days before becoming infectious to another mosquito. Completing this cycle takes two to three weeks. A seven-week chain indicates the cycle repeated at least twice, likely three times, without interruption.
The fourteen recorded cases likely represent only a fraction of the actual number, as approximately 75% of dengue infections produce no symptoms or symptoms too mild to prompt medical attention. Many more individuals in LA County may have been unknowingly infected.
The dengue virus transmission cycle. A mosquito bites an infected person, the virus replicates inside the mosquito over eight to twelve days, and the mosquito passes it to someone new.
CDC
A Connected World
Why did this outbreak occur in 2024? That year, LA County documented 222 travel-related dengue cases, a sharp increase from 35 in 2022 and 75 in 2023. In 2024, the Americas saw over 13 million cases, setting a new record. Each traveler returning to LA with active dengue viremia is a potential ignition point. With 222 such cases in a county where the primary mosquito vector, Ae. aegypti, has been present since 2013, the outbreak wasn’t unexpected.
This situation illustrates how global issues can become local challenges. LA County’s dengue problem arose not from a failure in mosquito control but due to a surge in cases globally, with infected individuals returning to an area where the vector was already present. The hantavirus outbreak on the cruise ship MV Hondius further underscores how quickly pathogens can spread with global travel.
Reported dengue cases in the Americas, 1980–2024. The 2024 total of nearly 13 million cases was three times the previous record set in 2023. Data: OpenDengue V1.2 (Clarke et al. 2024); 2024 total from PAHO.
John M. Drake
Climate change influences both ends of the spectrum, expanding the habitat and season for Aedes mosquitoes in temperate areas while increasing transmission in the tropics, contributing to the influx of infected travelers.
The Threshold Problem
Diseases naturally propagate. The distinction between no local dengue and some local dengue isn’t just about quantity; it’s a fundamental shift.
Below the transmission threshold, introductions of the virus die out naturally, allowing public health responses to be more measured due to favorable odds. Above the threshold, each infection can lead to more, compounding the problem and necessitating swift, coordinated responses in surveillance, diagnosis, and vector control, all of which are costlier than preventive measures.
Florida has gained insights over the past decade. Key West experienced its first modern dengue outbreak in 2009. Subsequently, Miami-Dade and other counties in South Florida began reporting sporadic local cases. By 2022–2023, Florida recorded over 60 local cases in a single season, managed through investments in surveillance, rapid diagnostics, and aggressive vector control.
California is earlier in this progression. The LA County investigation revealed a median of 10 days from symptom onset to dengue testing. One case was initially misdiagnosed as West Nile virus. Four out of the fourteen patients were identified by public health teams conducting door-to-door checks, rather than through the medical system. In a region where dengue isn’t endemic, diagnosis requires consideration by healthcare providers.
What Ended the Outbreak?
The dengue outbreak in 2024 concluded when mosquito activity ceased in late October. The timeline of the California outbreak shows a build-up of cases in August, September, and October before halting. The public health response was robust, involving 318 household surveys, nine field operations, and multilingual outreach. Whether these efforts alone could have ended the outbreak is uncertain, as the season ended first.
With climate change extending mosquito seasons, the global dengue burden is expected to grow. The pressure from introductions will increase, pushing systems already on the brink closer to their limits. Preventing the disease’s entry is nearly always more cost-effective than attempting to manage it once established.