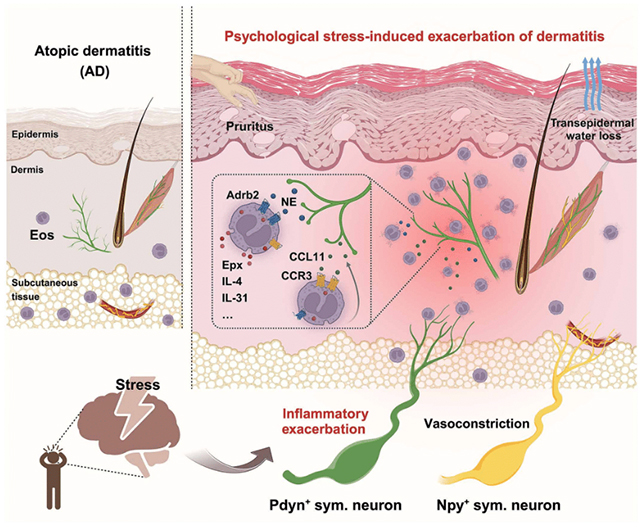
It has been recognized for some time that psychological stress can worsen eczema (atopic dermatitis), although the exact mechanism was unclear. Recent research may have identified the nerve pathway that explains this connection.
In studies using mouse models of eczema, scientists found a link between the nervous and immune systems involving a specific group of ‘fight-or-flight’ nerves located in the skin. Under stress, these nerves stimulate white blood cells known as eosinophils, which, while defending the body, can end up causing skin irritation.
This research, conducted by a team from Fudan University in China, suggests that their findings could enhance eczema treatments. Their results indicate that managing psychological stress could potentially reduce the severity of this skin condition.
The study began with 51 individuals with eczema, where researchers compared their reported stress levels with the severity of their skin inflammation and the presence of eosinophils. They observed a direct correlation between stress levels and eczema severity, primarily linked to elevated eosinophil levels in the blood and skin.
This prompted further investigation using mouse models. By exposing the mice to stress and employing advanced imaging and genetic analysis, researchers traced the connection between stress and eczema, mapping the brain’s stress centers to the skin.
This process initiates a sequence that starts with ‘fight-or-flight’ nerves, or sympathetic neurons, and culminates in exacerbated skin rashes, driven by eosinophils entering a more harmful state.

When mice were genetically altered to reduce eosinophil numbers, the link between stress and worsening skin rashes diminished, although eczema itself persisted. This aspect may be explored further in future research.
“These findings enhance our understanding of sympathetic neurons’ unique roles in skin inflammation, offering potential strategies for targeting specific neuronal subtypes in skin diseases,” write the researchers.
While eosinophils have previously been identified as contributors to eczema irritation, prior studies have not conclusively determined the efficacy of treatments targeting these immune cells.
The new findings imply that eosinophils play a role in how stress aggravates eczema, although they may not be the primary cause of the condition.
Related: Each Stressful Person in Your Life May Age You by Months, Study Finds
As much as 10 percent of adults are known to suffer from eczema, with atopic dermatitis being the most prevalent type. It can lead to skin pain, severe itching, and disrupted sleep, so any advancement in symptom relief would be beneficial.
In a linked commentary on this study, immunologists Nicolas Gaudenzio and Lilian Basso from the University of Toulouse in France propose that the brain may retain a ‘memory’ of previous eczema inflammation, which could be reactivated by stress.
These concepts warrant further research, with key questions still to be addressed, such as how this identified stress pathway may relate to other inflammatory conditions.
“The ways in which different types of psychological stress (acute or chronic, physical or emotional) activate the neuroimmune axis identified by the authors remain unclear,” Gaudenzio and Basso write in their commentary.
“Whether other immune or neuronal cell types are part of this process is also unknown. Exploring similar mechanisms in other stress-sensitive inflammatory diseases, like psoriasis or inflammatory bowel disease, is necessary.”
The research has been published in Science.