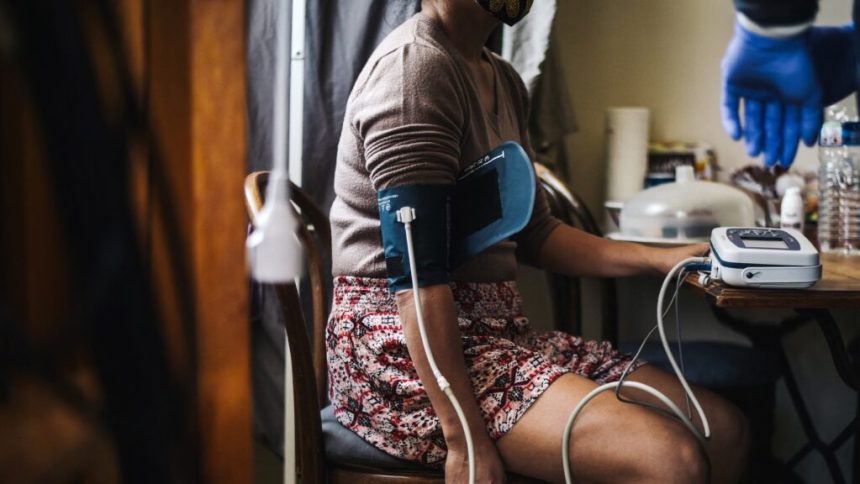
High blood pressure is a major contributor to heart attacks and strokes, making it a leading risk factor for mortality in the United States and globally.
Despite the availability of effective and affordable treatments, over half of Americans continue to suffer from uncontrolled hypertension, a condition exacerbated by negative social factors.
A recent study explored alternative solutions beyond traditional medication for low-income individuals with high blood pressure. The approach: a team-based, structured method involving home monitoring, feedback, medication adjustments, and health coaching by primary care providers, nurses, and community health workers.
The findings: patients receiving this approach had significantly lower blood pressure than those who received “enhanced” standard care at 36 federally qualified health centers in Louisiana and Mississippi. The study spanned 18 months and coincided with the onset of the COVID-19 pandemic, which disrupted healthcare services.
Dan Jones, a cardiologist involved in creating the American Heart Association’s latest blood pressure guidelines, praised the study as a significant advancement in blood pressure management.
“This method applies team-based care in some of the most challenging clinical environments in the U.S.: federally qualified community health centers in two of the poorest states,” he explained to STAT. Jones, a former president of the American Heart Association and dean emeritus of the University of Mississippi School of Medicine, was not part of the research. “They faced unplanned hurdles due to the pandemic but managed to prove their point effectively.”
Historically, maintaining a systolic blood pressure below 140 mm Hg was the target. However, findings from the Systolic Blood Pressure Intervention Trial (SPRINT) revealed that reducing it to below 120 mm Hg significantly decreases the risk of heart attacks, heart failure, strokes, and overall mortality.
The study, published in the New England Journal of Medicine, marks the first randomized controlled trial to implement this intensive strategy aimed at improving hypertension control among low-income patients, as described by co-author Jiang He, chair of epidemiology and professor at UT Southwestern. This approach is rooted in the SPRINT trial principles.
Teams adjusted care and medications, patients monitored their blood pressure at home and reported their readings at least three times weekly for feedback, while community health workers helped patients maintain their medication regimen and adopt lifestyle changes.
Over 1,200 patients with uncontrolled hypertension were divided into two groups. One group received standard care, seeing a physician every four to six months. The other underwent the SPRINT team approach, with monthly visits for medication adjustments. Most participants were already on blood pressure medications, with an average age of 59. Slightly more than half were women, nearly two-thirds were African American, three-quarters were unemployed, and a similar proportion had a family income under $25,000 annually.
Co-author He noted that it was difficult to ensure patients attended regular visits and afforded their medications.
“Many patients have to decide between buying food or medicine due to limited resources,” he said.
Health coaches, including nurses or medical assistants, assisted patients in applying for medication assistance programs to help them afford and adhere to their treatments.
Over 18 months, patients in the team-supported care group saw an average reduction of 16 mm Hg in their systolic blood pressure, compared to a 9 mm Hg reduction in the control group. The team group also demonstrated better adherence to their blood pressure management plans, with similar serious side effects reported by both groups. The average cost of implementing the team approach was $762 per patient.
Marie Krousel-Wood, associate provost for the health sciences at Tulane University, stated that these results align with other studies at Kaiser Permanente and Veterans Affairs, which employed similar system-level interventions. “This approach, tested in rural and urban clinics among low-resourced and underserved populations, resulted in lower blood pressure compared to the control group, even for patients already on medication but still experiencing uncontrolled hypertension,” she noted.
Tom Frieden, president and CEO of the nonprofit Resolve to Save Lives and a former CDC director, commended the trial for applying SPRINT findings to the most beneficial groups. He emphasized that even minor investments in enhanced care can yield positive results.
“The key issue is why the U.S. healthcare system struggles with blood pressure control, which can prevent more deaths than any other clinical intervention,” he commented via email to STAT, highlighting the gap between prevention and treatment. “Many in American healthcare see a heart attack as a revenue-generating event. Until this changes, trials like this will remain isolated successes.”
An editorial accompanying the NEJM study highlighted the need for systems-based strategies in community health centers. It described the blood pressure differences between the intervention and control groups as “modest” and noted the associated costs.
“We must do better for our patients and communities by bridging the gap between evidence-based therapies and routine clinical practice to enhance blood pressure control and improve cardiovascular, kidney, and brain health,” wrote Sadiya Khan from Northwestern University and Mark Huffman from Washington University School of Medicine.
Study co-author He responded, “In this low-income population, we achieved blood pressure control with systolic levels below 130 mm Hg in 47.7% of patients, compared to 22% in the general U.S. population, indicating significant public health implications.”
The researchers aim to expand the study beyond Louisiana and Mississippi and perform an economic analysis. Jones hopes the findings will inspire systemic changes in healthcare.
“This is not a decision an individual physician or clinician can make alone,” he said.
STAT’s coverage of chronic health issues is supported by a grant from Bloomberg Philanthropies. Our financial supporters are not involved in any decisions about our journalism.