While Alzheimer’s disease is often seen as an age-related illness, the brain changes associated with it actually begin much earlier, around the third decade of life.
Initially, a tangled form of a protein known as tau starts accumulating in a small, deep brain region involved in sleep, attention, and alertness called the locus coeruleus. Subsequently, tau spreads throughout the brain.
The presence of tau tangles does not necessarily indicate Alzheimer’s disease, as they occur to varying extents in nearly everyone. However, because these changes originate in the locus coeruleus, some brain researchers, including myself, consider this area a warning sign for Alzheimer’s development.
We are investigating whether halting or slowing tau tangles in this brain region, or maintaining its health, might interrupt the disease’s progression and prevent other aspects of cognitive aging.
Recent research from my lab and others is exploring the potential of a therapy called vagus nerve stimulation, already used for various health conditions, to help maintain the locus coeruleus’s proper function.
The locus coeruleus and Alzheimer’s disease
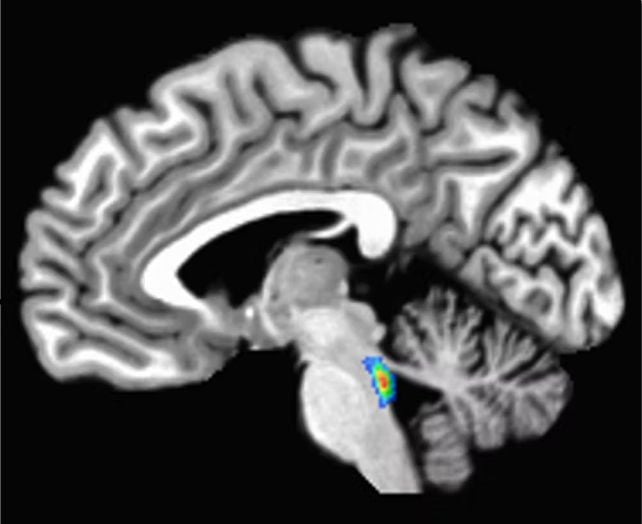
The locus coeruleus is located in the brain stem, the brain’s lowest part. Its name, meaning “blue spot,” is derived from a pigment called neuromelanin produced by its cells.
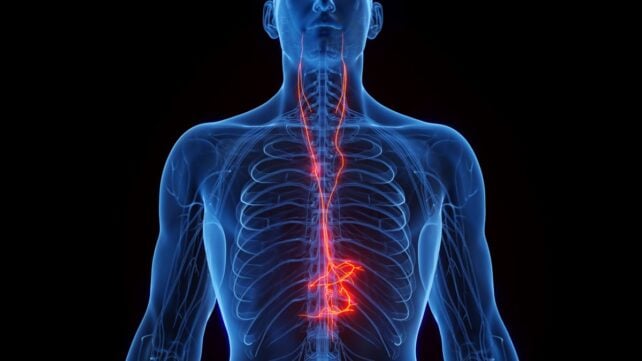
The locus coeruleus is vital for various fundamental human functions. It produces almost all of the brain’s norepinephrine, a chemical essential for sleep, alertness, focus, learning, and even immune function.
It also receives signals from nerves throughout the brain and body, including the vagus nerve, which transmits information to and from the heart, lungs, and other organs.
My research examines this brain region’s structure, how nerve cells transmit messages within it, and how it connects with other brain regions. I also study how these features evolve over time and impact cognition and memory.
 frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>
frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>Research indicates that from middle age onward, nerve cells in the locus coeruleus might be damaged by tau accumulation. This damage could be linked to memory decline. Tau buildup, cell death, and reduced function in the locus coeruleus precedes and predicts Alzheimer’s diagnosis and symptoms.
These insights have led researchers to propose that maintaining the health of the locus coeruleus might help protect the entire brain.
Vagus nerve stimulation and brain health
The vagus nerve facilitates communication between the brain and organs in the chest and abdomen, such as the heart and intestines. It helps the brain monitor and manage several of the body’s critical organs and sends rest and digest signals, promoting digestion and cellular repair.
In the 1980s and 1990s, researchers found that stimulating the vagus nerve could alleviate epilepsy. They also discovered additional benefits, such as enhancing mood and cognition.
Currently, the Food and Drug Administration approves vagus nerve stimulation for not only epilepsy treatment but also for migraine and depression, as well as assisting with stroke recovery.

Vagus nerve stimulation for epilepsy and depression usually involves implanting an electrical stimulator on the left side of a patient’s chest, where the vagus nerve is located. Noninvasive devices for treating headaches apply gentle electric pulses to certain neck or ear areas where the vagus nerve is near the skin’s surface.
Before identifying the locus coeruleus’s connection to Alzheimer’s disease, researchers speculated that vagus nerve stimulation might enhance mood and cognition in affected individuals. This is partly because vagus nerve stimulation might elevate brain norepinephrine levels, which are deficient in Alzheimer’s patients.
Maintaining balance
Neuroscientists are still uncertain about how vagus nerve stimulation benefits the brain, but one prominent theory is that it helps regulate nerve cell activity in the locus coeruleus, allowing it to function effectively.
Excessive activity in the locus coeruleus could make individuals overly alert, causing stress or panic. In fact, a hyperactive locus coeruleus contributes to some post-traumatic stress disorder symptoms. Conversely, insufficient activity might lead to depression or memory challenges.
Some vagus nerve stimulation methods do not increase or decrease locus coeruleus activity but instead influence the timing and rhythm of neuron firing. Other methods appear to boost norepinephrine levels in rats’ brains, and researchers believe this might also explain how vagus nerve stimulation treats epilepsy.
Related: Vagus Nerve Stimulation Has Lasting Effects in People With Severe Depression
These findings suggest that vagus nerve stimulation might effectively regulate the locus coeruleus, ensuring it maintains the optimal level of activity for proper functioning.
Can vagus nerve stimulation combat memory loss?
There are emerging indications that vagus nerve stimulation might benefit the aging brain.
Some studies have shown that vagus nerve stimulation can prevent memory deterioration or even enhance it in individuals with mild cognitive impairment or at the early stages of Alzheimer’s disease.
In a trial involving 52 participants aged 55 to 75 diagnosed with mild cognitive impairment, significant improvements in memory and overall cognition were reported after undergoing vagus nerve stimulation for an hour daily, five days a week, over approximately six months.
Research conducted on healthy adults around age 60 and healthy adults aged 18 to 25 has also reported memory improvements after a single session of vagus nerve stimulation.
Although this research is still in its early stages, it offers hope for a potential new approach to managing some of the challenging symptoms associated with Alzheimer’s disease and aging.![]()
Elizabeth Riley, Lecturer in Psychology, Cornell University
This article is republished from The Conversation under a Creative Commons license. Read the original article.