A new study indicates that the rising frequency of droughts due to global climate change could be fostering ideal conditions for the evolution of antibiotic-resistant bacteria.
While the excessive use of antibiotics in medicine has long been recognized as a driver for resistant bacteria, this research highlights that environmental factors, particularly in the Earth’s soil, may also play a crucial role in influencing antibiotic resistance within healthcare environments.
Researchers from the California Institute of Technology (CIT) have discovered that drought conditions can concentrate natural antibiotics in soil, thereby encouraging microbes to develop antibiotic-resistant genes.
As climate change causes droughts to become more frequent, severe, and widespread, microbes equipped with genetic adaptations to withstand these concentrated soil antibiotics are thriving.
Historically, bacteria in soil have produced antibiotics as a means to outcompete other microbes. This practice predates the use of antibiotics in human medicine.
“Similarly, antibiotic-resistant bacteria and the genes responsible for this resistance have existed long before human medicine, evolving as natural defense mechanisms against antibiotic-producing bacteria,” explains microbial ecologist Timothy Ghaly from Macquarie University in Australia, who provided commentary on the study.
Ghaly poses an important question: “What environmental factors could facilitate the transfer of antibiotic resistance genes from soil bacteria to clinical human pathogens?”
To explore this, the CIT researchers examined five datasets from soil samples collected in the USA, China, and Europe, assessing the impact of drought on soil microbial communities across various environments such as cropland, grassland, forests, and wetlands.
All five datasets showed that drought conditions coincided with an increase in genetic material from antibiotic-producing bacteria and genes known for antibiotic resistance.
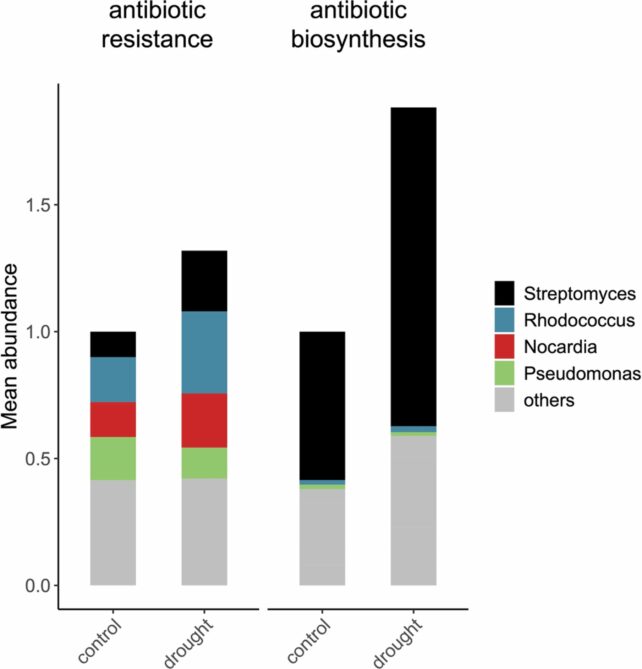
This means that bacteria in drought-stricken soil samples are more adept at surviving antibiotic exposure.
In related lab experiments, researchers introduced an antibiotic to a small-scale soil ecosystem and simulated drought by drying it out. This increased the antibiotic’s concentration in the soil.
Bacteria species already resistant to the antibiotic fared equally well in both dry and damp soils, whereas those sensitive to the antibiotic mostly perished in the drought-like conditions.
The surviving bacteria included antibiotic producers, which are naturally resistant to their own compounds, leading to an increase in both antibiotic producers and resistant bacteria in the soil.
“By establishing the role of drought in enhancing antibiotic resistance in soil, the researchers make a concerning link between this natural phenomenon and global public health,” Ghaly explains.

An analysis of hospitals in 116 countries revealed a strong correlation between antibiotic resistance inside hospitals and the local aridity index, which measures climate dryness.
This correlation persisted even after accounting for national income, which can influence antibiotic usage and healthcare systems.
“This suggests a fundamental driver of clinical resistance through a global environmental mechanism, where climatic conditions in natural ecosystems affect pathogen evolution in human environments and ultimately human health,” writes Ghaly.
Related: Ancient Killer Is Rapidly Gaining Resistance to Antibiotics, Scientists Warn
Although the evidence is not definitive enough to claim that droughts are increasing antibiotic resistance in clinical settings, it does imply that climate change, particularly the droughts it exacerbates, may heighten the risks.
“Our study offers a clear example of how climate change has the potential to intersect with microbial ecology to shape public health outcomes, highlighting the importance of integrating environmental and clinical perspectives,” the authors conclude.
“As climate instability intensifies, such integrative approaches will be crucial for anticipating and mitigating the global trajectory of antibiotic resistance,” they add.
The research is published in Nature Microbiology.





